Linda T., 54, from Springfield, Missouri, used to keep a running list on her phone. Heart palpitations at 2 a.m. A stomach that locked up without warning. A low-grade dread that settled into her chest every single morning before she even got out of bed. Ringing in her ears. Exhaustion that sleep did not fix.
She had been to eight different doctors in four years. She had a clean EKG. A normal Holter monitor. A colonoscopy that found nothing. Three therapists, two of whom had put her on anti-anxiety medication. The medication made the anxiety quieter but it never made it go away. It also made her feel like she was watching her own life through a slightly foggy window.
"I started to believe I was just falling apart," she said. "Like my body had turned against me for no reason."
What none of those eight doctors had done was take an X-ray of her cervical spine.
Key finding: Research in cervicogenic disorders documents that upper cervical dysfunction can produce systemic symptoms far beyond neck pain, including autonomic dysregulation affecting the heart, digestion, and stress response. Most patients spend years in the specialist system before anyone looks at the neck.
$119.99 (Was $239.98) | 30-Day Money-Back | Free US Shipping
The Anatomy Nobody Talks About
A physical therapist specializing in cervicogenic disorders describes it this way:
"Most patients have never heard of the vagus nerve. That's part of the problem. It is the tenth cranial nerve, and it is one of the longest nerves in the human body. It exits the brainstem, passes through the jugular foramen at the base of the skull, and travels directly alongside the C1 and C2 vertebrae as it descends through the neck. From there it reaches the heart, the lungs, the stomach, the intestines, and the immune system."
Physical therapist specializing in cervicogenic disorders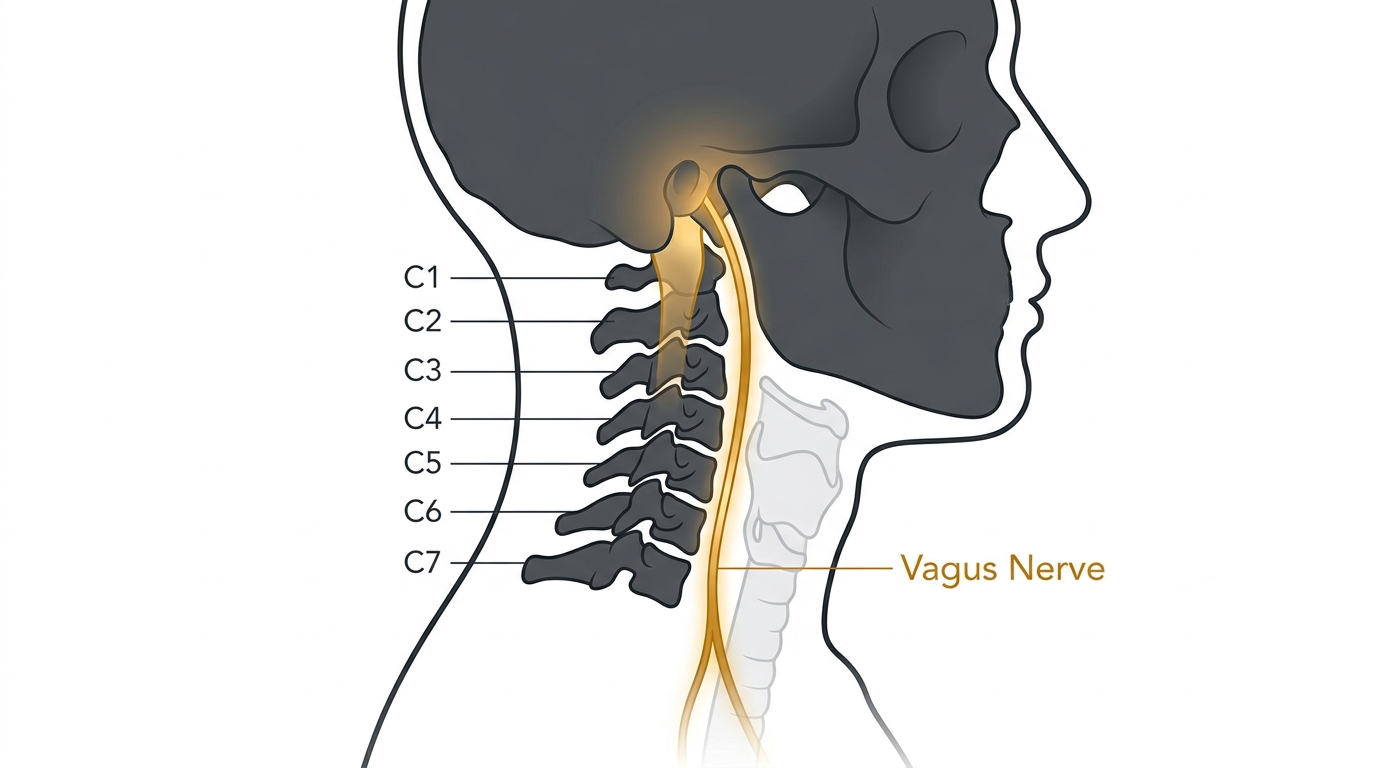
"This nerve is the primary highway of the parasympathetic nervous system, the system responsible for what people call 'rest and digest.' It regulates heart rate variability, controls the rate of digestion, modulates the immune response, and plays a central role in the body's ability to feel calm rather than threatened."
Physical therapist specializing in cervicogenic disordersWhen the cervical spine loses its natural 26-degree curve, and this happens gradually, often from years of forward head posture, screen time, or a minor injury that was never properly rehabilitated, the surrounding muscles go into chronic low-grade spasm. Those muscles sit millimeters from the vagus nerve. When they tighten, they compress it.
Heart rate that flickers irregularly. Digestion that stalls. A nervous system that cannot get out of fight-or-flight regardless of how calm the patient's life actually is. Unexplained fatigue, brain fog, and a constant low-level anxiety with no identifiable psychological trigger.
The Medical System's Blind Spot
The reason this goes undiagnosed for years has less to do with incompetence than with how modern medicine is organized.
A cardiologist looks at the heart. When the EKG is normal, the patient is cleared. The cardiologist does not order a cervical X-ray because cervical spines are not within the scope of what she treats. A gastroenterologist looks at the gut. When the colonoscopy is normal, the patient is cleared. She does not ask about neck posture. A psychiatrist or therapist looks at psychological causes of anxiety. When the patient has no obvious trauma and no identifiable trigger, the diagnosis becomes generalized anxiety disorder. The prescription pad comes out.
Nobody is asking: what nerve connects all of these systems? Nobody is asking: where does that nerve go?
"Overspecialization is one of the most underappreciated diagnostic failures in modern medicine. Every specialist is an expert in one branch. The vagus nerve doesn't care about branches. It runs through all of them."
Physical therapist specializing in cervicogenic disordersLinda's Turning Point
Linda found a physical therapist by accident. She had strained her shoulder moving boxes, and her GP referred her to a local PT clinic. During the intake exam, the therapist noticed something she had not been looking for: Linda's head was positioned roughly an inch forward of where it should be. Her cervical curve was nearly flat on the lateral view X-ray.
"She asked me about all of these other symptoms that seemed totally unrelated to my shoulder," Linda recalled. "The heart stuff, the stomach stuff, the anxiety. I thought she was being weird. And then she explained the vagus nerve to me. I literally sat there with my mouth open."
The therapist began working on cervical traction: manually decompressing the upper cervical joints, mobilizing C1 and C2, and reestablishing the natural curve. Within two weeks, Linda's resting heart rate had stabilized. Within a month, the morning dread she had lived with for four years was noticeably quieter. The stomach locking stopped.
"I have been on and off anti-anxiety medication for three years. Two weeks of cervical work did more than any of it."
Linda T., 54, Springfield, MissouriWhy the Neck Is Almost Never Checked
The vagus nerve sits deep in the neck, shielded by muscle and fascia. Its compression does not produce neck pain in most patients. It produces systemic dysregulation: symptoms that look like organ disease, cardiac disease, or psychiatric illness. This is why it takes an average of several years and multiple specialists before a patient with vagus nerve compression gets a correct explanation.
The symptoms are real. The organ tests are normal. The gap between those two facts tends to be filled with a psychiatric diagnosis.
Cervical traction, the mechanical restoration of the neck's natural 26-degree curve, is the oldest and most clinically documented treatment for upper cervical disorders. It decompresses the joints at C1-C2, reduces the muscle spasm pressing on the nerve, and allows the vagus nerve to conduct signals without interference. A single session of clinical cervical traction at a physical therapy office costs between $80 and $150. Most patients require 12 to 24 sessions to see lasting results.
Neckline 4-in-1 Massager
Clinical-grade cervical traction for daily home use
- 26° cervical traction incline (same angle used in PT clinics)
- Deep heat therapy to reduce muscle spasm around the vagus nerve
- EMS electrical muscle stimulation to interrupt tension cycles
- Targeted massage along suboccipital muscles and upper trapezius
- 15-minute daily protocol
- 30-Day Money-Back Guarantee
$239.98 $119.99 Spring Sale
The At-Home Cervical Traction Solution
The Neckline 4-in-1 Massager is not a neck massager that happens to support the neck. It is a cervical traction device built around the specific 26-degree incline that clinical cervical traction uses to decompress the upper cervical joints. The incline creates gentle axial decompression, the same mechanical force a physical therapist applies manually.
The four components work together:
26-degree cervical traction incline. The structural component. The neck rests at the precise angle used in clinical traction protocols. The weight of the head creates gentle, consistent decompression at C1-C2. This is the mechanism that addresses vagus nerve compression at the source.
Deep heat therapy. Heat penetrates the muscles surrounding the vagus nerve pathway, reducing the chronic low-grade spasm pressing on the nerve. Clinical traction sessions typically combine traction with heat for exactly this reason.
EMS (electrical muscle stimulation). EMS signals the muscles to contract and release in a controlled rhythm, interrupting the chronic tension cycle. The same technology is used in professional PT clinics.
Massage function. Targeted mechanical massage along the suboccipital muscles and upper trapezius: the muscles most directly associated with upper cervical compression.

Linda's Results: Week by Week
Linda T. — Progress Timeline
What Users Are Saying
"I had been diagnosed with generalized anxiety disorder at 49. I was on medication for two years. My functional medicine practitioner finally suggested we look at my cervical spine. Flat curve. I started doing cervical traction at a PT office, then found the Neckline for home use. Within six weeks my heart rate variability improved measurably on my smartwatch. I tapered off medication over four months. This is not a magic device. But it addressed something the medication never did."
"The vagus nerve explanation was the first thing in five years that made my symptoms make sense. Racing heart, bad digestion, constant low-level anxiety, and neck pain that I always just thought was stress. My chiropractor had mentioned cervical curve issues but never connected it to any of this. I use the Neckline every night. The palpitations are mostly gone. The stomach issues are maybe 80% better. I wish I had known about this years ago."
"I am 57 and I spent three years thinking I had some combination of anxiety disorder, IBS, and a heart arrhythmia. Clean tests everywhere. My therapist actually suggested I look into cervicogenic dysfunction after she had seen a few other patients with similar patterns. The Neckline is now part of my daily routine. Not an exaggeration: most of my symptoms are gone. What remained turns out to have been actual anxiety, just much less of it than I thought."
